
The Long-Term Effects of an Untreated Hepatitis C Infection
Hepatitis C is a virus that causes ongoing inflammation of the liver. Transmitted through the blood, it’s known as a “silent virus” because it can live in the body for years or even decades without causing symptoms. There’s no vaccine for hepatitis C, but treatment has greatly improved over the years.
Hepatitis C virus (HCV) is most commonly spread through unsterile needles. If you believe you may have been exposed to Hepatitis C or are at increased risk of contracting the virus (especially if you are an IV drug user or were born between 1945 and 1965), see a primary care physician as soon as possible.
Acute vs. Chronic Hepatitis C
Hepatitis C infection can be acute, short-term, or chronic, lifelong.
- Acute Hepatitis C occurs within six months of exposure to the virus. HCV can be a short-term infection that the body clears on its own, but most people will go on to develop a chronic infection.
- Chronic Hepatitis C can last for years, decades, or even a lifetime. If left untreated, HCV can lead to serious health complications, including liver damage, scarring of the liver (cirrhosis), liver cancer, and even death.
Approximately 75%–85% of HCV infection cases become chronic.1 In about 15%–25% of cases, a person’s body will rid itself of the virus on its own without treatment; this is called spontaneous clearance, and experts aren’t sure exactly sure why it happens.1
Experts also aren’t sure why so many cases of hepatitis C infection become chronic. It might be due to changes that occur as the virus replicates; these changes may protect the virus against attacks by the immune system.
How Common Is Hepatitis C?
The Centers for Disease Control (CDC) estimates that 2.4 million people in the U.S. are living with hepatitis C.
In 2016, just under 3,000 cases of acute hepatitis C were reported, but experts believe hepatitis C infections are significantly underreported.1 The number of acute cases is estimated to be nearly 14 times higher than reported. That would put the number of HCV cases in 2016 closer to 41,000.1
Risk Factors
Most cases of hep C transmission occur from sharing needles or other equipment used to inject drugs. Before 1992, hepatitis C was also spread through blood transfusions and organ transplants.1 Today, the country’s blood supply is screened for hepatitis C, which has nearly eliminated this source of infection.

Your risk of getting hepatitis C is higher if you:
- Have ever injected or inhaled illicit drugs (e.g., heroin)
- Have HIV
- Are a healthcare worker who has had a needlestick injury or was otherwise exposed to infected blood
- Received a tattoo or body piercing with unsterilized equipment
- Were born to a woman with a hepatitis C infection
- Have ever been in prison—read more about hepatitis C and incarceration2
- Received a blood transfusion or organ transplant before 1992
- Were born between 1945 and 1965
- the rate of hepatitis C among people in this age group, “baby boomers”, is five times higher than those born in other years3
You can’t get or spread hepatitis C by sharing eating utensils, breastfeeding, kissing, coughing, or sneezing.
It’s uncommon, but not impossible, to get hepatitis C by sharing personal care items that have come into contact with an infected person’s blood, such as a shaving razor.
It’s also less common to get hepatitis C through sexual contact but having HIV or a sexually transmitted infection (STI) puts you at greater risk.
Signs and Symptoms of Hepatitis C
People with acute (new) hepatitis C infection usually don’t have symptoms. When symptoms do appear, they typically develop within two to twelve weeks of becoming infected.1 Symptoms may include:
- Fever
- Abdominal pain
- Nausea
- Vomiting
- Loss of appetite
- Dark urine
- Clay-colored stools
- Joint pain
- Jaundice (yellow skin or eye whites)
It’s important to know that you can spread the infection to someone else even if you have no symptoms.
Complications
Chronic hepatitis C infection can be serious and lead to long-term health complications. These include:
- Buildup of toxins in the brain: Liver inflammation can lead to liver failure, which can cause toxins to build up in the brain. This can lead to mental confusion, moodiness, and slurred speech.
- Jaundice: When HCV affects liver function, it can lead to jaundice, a yellowing of the skin and whites of the eyes caused by high levels of bilirubin.
- Fatigue and sluggishness: Hepatitis C infection can cause your immune system to mistakenly attack thyroid cells, which can lead to overactive and underactive thyroid function; these conditions can lead to fatigue and sluggishness.
- Nutrient absorption problems: When HCV causes significant liver inflammation, it can prevent your intestines from properly absorbing vitamins, minerals, and nutrients from food. Nutrient deficiency can lead to hair loss, dry skin, and weak fingernails. It can also lead to weight loss. Disruption of the digestive system can make it hard for the body to eliminate waste products, which can cause abnormally dark urine and/or clay-colored stools.
- Scarring of the liver (cirrhosis): Chronic inflammation can cause your liver to become scarred over the course of decades; this can make it difficult for your liver to function properly. Hep C infection is a leading cause of cirrhosis. 10%-20% of people infected with hepatitis C virus will develop cirrhosis over 20-30 years.1 You’re more likely to develop cirrhosis if you have hepatitis C infection and are male, over the age of 50, use alcohol, have nonalcoholic fatty liver disease, or take immunosuppressive drugs.
- Liver failure: Advanced cirrhosis can cause your liver to stop functioning; 3%-6% of people with HCV will develop liver failure.1 You may need a transplant if your liver fails.
- Liver cancer: While rare, hepatitis C infection can cause cancer or the liver; 1%-5% of people with HCV will develop liver cancer.1
Diagnosis
Doctors use a blood test to screen for hepatitis C virus. You should be screened for HCV if you have any of the risk factors mentioned earlier (see “Risk Factors” section above).
If an initial blood test is positive for hepatitis C, your doctor will likely order additional blood tests to measure the viral load—that is, the quantity of hepatitis C virus in your blood.
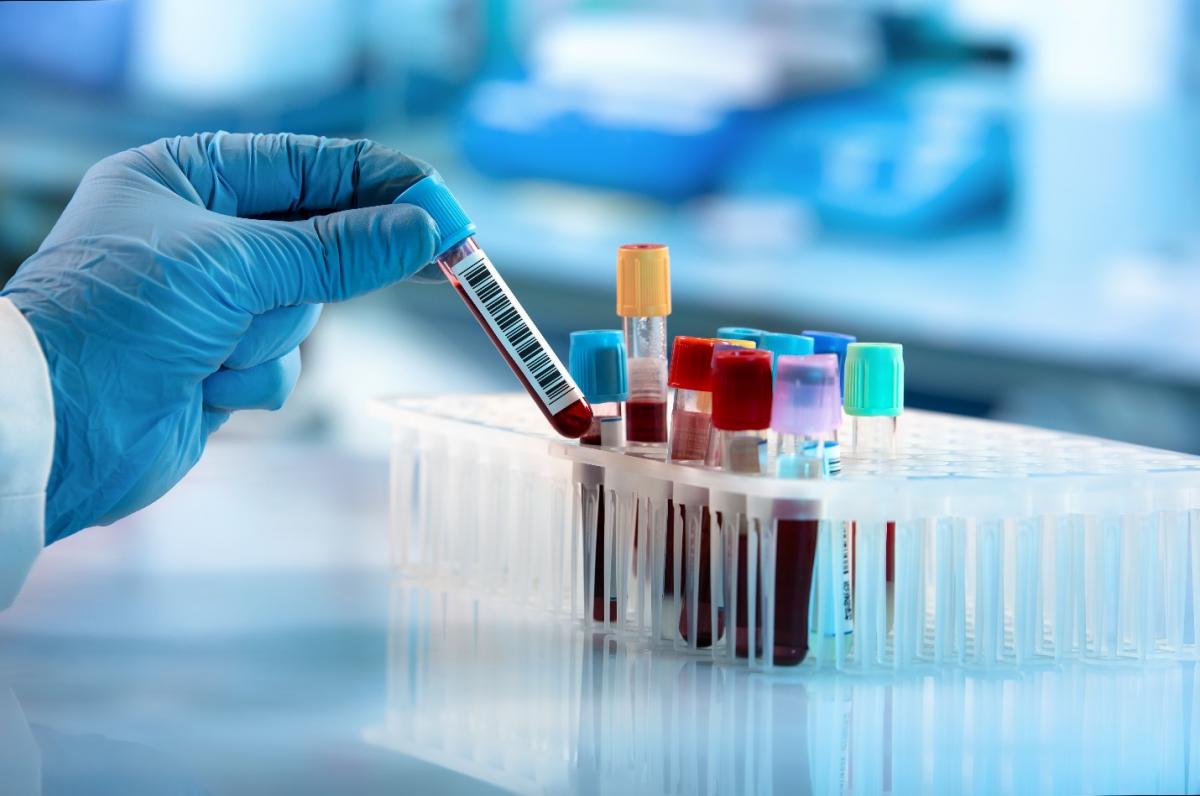
Additional blood tests can help the doctor determine the specific genotype (strain) of HCV. This is important for determining which treatment is best.
If you have chronic HCV, your doctor may order additional tests to determine if you have liver damage. These may include:
- Magnetic resonance elastography (MRE): This test combines magnetic resonance imaging (MRI) technology with a tool that detects sound wave formation to create a visual “map” showing the condition of your liver.
- Transient elastography: This test is a type of ultrasound that measures how fast vibrations travel through the liver; this can help the doctor estimate how stiff your liver tissue is because stiff liver tissue indicates scarring.
- Liver biopsy: This test involves removing a sample of liver tissue for lab testing; it’s done using a thin needle through the abdomen.
Hepatitis C Treatment
Hep C treatment depends on the stage of the disease:
Acute Hep C Infection
- There is no recommended treatment for acute hepatitis C. Your doctor will likely recommend being tested periodically to see if the infection clears on its own.
Chronic Hep C Infection
- Antiviral Medications: If you have chronic hepatitis C, your doctor may recommend antiviral medications to clear the virus from your body. Researchers have made significant progress recently in creating “direct-acting” antiviral drugs. These medications have fewer side effects and shorter treatment times, typically 8-12 weeks. Which medication your doctor chooses will depend on your specific profile—which virus genotype you have, whether you have existing liver damage, and your medical history and prior hepatitis treatments.
- Liver transplantation: If you have serious complications from chronic hepatitis C infection, your doctor may recommend liver transplantation. A liver transplant doesn’t cure hepatitis C, and the infection may return and require treatment with antiviral medications to clear the virus and prevent damage to the new liver, but a liver transplant can be a lifesaving procedure for those who need it.
- Vaccines: There is no vaccine for hepatitis C, but your doctor may recommend vaccines for hepatitis A and B viruses, which can also cause liver damage and worsen hepatitis C.
Lifestyle Changes and Home Remedies
If you’re diagnosed with hepatitis C, your doctor may recommend certain lifestyle changes to keep you healthy longer. He or she may recommend that you:
- Stop drinking alcohol, which can contribute to liver damage.
- Avoid certain medications, including over-the-counter (OTC) medications and herbal supplements that may cause liver damage; your doctor will counsel you on which medications and supplements to avoid.
- Protect others from coming into contact with your blood by using condoms, telling your partner about your HCV status before you have sex, covering open wounds, and avoiding donating blood, body organs, or semen.
Hepatitis C Prevention
Hepatitis C is most commonly spread through needles. To reduce your risk of getting it:
- Avoid injecting drugs. But, if you do, always use sterile injection equipment and avoid reusing or sharing needles.
- Practice safer sex. That means not having unprotected sex with multiple partners or with a partner whose health status you’re not sure about.
- Be careful about tattooing and body piercing. Look for a clean, reputable shop. Make sure the employees use sterile equipment by asking questions. If the employees won’t answer your questions or you have concerns about the shop, listen to your gut and look for another shop.

Taking Control of Your Health with Hepatitis C Screening and Treatment
Hepatitis C may be known as a “silent virus,” but there are things you can to do protect your health, whether you’ve been diagnosed with HCV or you’re in a high-risk group for HCV infection. If you’re unsure of your status, your first step is getting screened.
The primary care physicians at Crystal Run Healthcare provide world-class care in state-of-the-art facilities. They act as your first point of contact and will work with you to schedule appropriate screenings and coordinate your care with our renowned team of specialists.
Contact us today to schedule a consultation with one of the general practitioners on our team.
Sources:

 Optum Radiology at Crystal Run Healthcare
Optum Radiology at Crystal Run Healthcare Same and next-day pediatric appointments
Same and next-day pediatric appointments